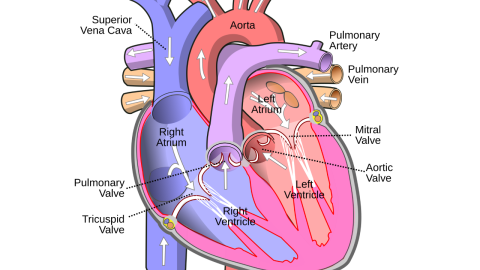
Your recovery at home after cardiac surgery

Information and resources to help you with your recovery at home after cardiac surgery.
What to expect
Recovery usually takes eight to 12 weeks, but you will get better at your own rate. Many things affect how quickly people recover. These include how active people are before surgery, their kind of surgery, and their age. Even when you are ‘healed,’ it can still be several months before you feel completely recovered.
When you get home, you might be surprised by how tired you feel. This feeling is normal. Your energy level will improve over the next few weeks. Things you can do to help with your recovery include:
- Keep your pain manageable
- Take care of your incision
- Eat a balanced diet
- Go for daily walks
- Rest and relax
- Take your medications as prescribed
- Share your emotions and feelings
Emotions and feelings
After surgery, you might feel “blue” or in low spirits. This may start in the hospital or after you go home. This is common and may last a few days or weeks. Family members may also feel a range of emotions.
Each person's recovery is unique, and there is no right or wrong way to cope. You may find that sharing and discussing your concerns with your family members, friends, or primary care provider is helpful. You may also find attending a support group helpful. Ask your primary care provider or surgeon about any support groups that may be available.
See your primary care provider if you, your family members or friends are concerned that your mood is affecting your recovery (i.e., interfering with your sleep, exercise, and appetite).
When to contact your doctor
Contact your surgeon or primary care provider, or go to the Emergency Department if any of the following happen:
- Your pain gets worse or does not go away with pain medication
- You have a fever of 38.0° C (100.4° F) or above
- Your incision comes apart or becomes red, swollen, or hot to the touch
- You notice foul-smelling liquid coming from your incision
- You start bleeding from your incision
- You have difficulties with swallowing, resulting in a decreased appetite and constant weight loss
- You feel sick to your stomach (nauseated) or throw up (vomit) often for more than 24 hours
- You have diarrhea that lasts for more than two days
- If you experience any pain, aching or redness in your calves or swelling of the legs
- You have difficulty breathing
If you cannot contact your surgeon or primary care provider, go to the nearest Emergency Department or call HealthLink BC at 8-1-1 to talk to a registered nurse. Be sure to tell them about your recent surgery.
Rest and activity
Keeping active is one of the best ways to keep healthy and recondition your heart muscle. Activity also helps build strength, improves circulation, and makes you feel better.
Attending a cardiac rehabilitation program after discharge is recommended to help support your recovery.
Pain management
You must take your pain medication regularly (e.g. before activity and/or bedtime) to help your overall recovery, to ensure you can:
- be comfortable enough to sleep
- get out of bed
- participate in daily activities inside and outside the home.
The goal is to take the least amount of medication, which will limit the side effects you may experience. If you are using a traditional medication, let a health-care team member know in case there are any concerns.
It is normal for you to have some pain for the first few weeks after you leave the hospital. As your incision heals, there can be chest wall numbness and/or burning, prickling and sensitivity at the incision site. This is related to your body healing and the nerves repairing themselves. These sensations will go away over time as your body heals.
How to manage your pain
- Use a pillow for support during your deep breathing and coughing exercises.
- Try non-medication therapy such as warm or cold compresses, positioning, imagining peaceful situations, and listening to music.
- First, try taking acetaminophen (Tylenol®).
- If Tylenol® alone is not enough to ease your pain, ask your primary care provider if pain medication such as ibuprofen (Advil, Motrin) or another non-steroidal anti-inflammatory (NSAID) medication is an option.
- If you’ve been prescribed opioid pain medication (e.g. hydromorphone, oxycodone), take this medication if the Tylenol® and ibuprofen do not help.
Opioid pain medication
Opioid medications are sometimes called “narcotics.”
Commonly prescribed opioids include:
- Codeine: Tylenol 3.
- Tramacet/Tramadol.
- Oxycodone.
- Hydromorphone: Dilaudid.
Information on opioid pain medication
-
Can I get addicted to opioid medications?
When you take opioid medication for acute pain, such as the pain that happens after operations or accidents, the risk of addiction is low.
Taking opioid medication for an extended time can lead to dependence. It is important to taper off opioid medication as your pain improves.
Some people may be at higher risk for developing an addiction to opioid medication. Your health-care team will discuss this with you and develop a plan for tapering off the opioid medication.
-
What are the side effects of opioid pain medication?
- Confusion
- Nausea
- Vomiting
- Constipation
- Sleepiness
- Itchiness
- Inability to urinate
- Slowed breathing
Opioid pain medication can impair driving and the ability to use power tools or operate machinery. It would be best to avoid these activities until you no longer take opioids. Always read and follow any instructions provided with your medications. If you have questions, discuss them with your practitioner or pharmacist.
-
When do I start tapering off opioid medication?
When the surgical pain becomes manageable, you should reduce how many opioids you take.
-
How do I taper off opioid medication?
-
Reduce how much you are taking (the number of pills you take). For example, if you were taking two pills each time, start taking one pill to see if the pain is managed. If it is, continue with one pill each time. Do this for one to two days.
-
Then, reduce how often you are taking the medication. For example, if you were taking a dose every four hours, then take a dose every six hours instead for one to two days. Then, take a dose every eight hours for one to two days. Then consider stopping.
-
-
Can I go through withdrawal?
Withdrawal symptoms are a sign that your body is used to taking opioids regularly and that you need to taper off the opioids more slowly.
Withdrawal symptoms are:
- Sweating
- Fever
- Nausea
- Vomiting
- Feeling agitated or irritable
-
How do I store opioid medication?
These medications should be kept out of sight and ideally in a hidden or locked area.
Make sure you keep your opioid medications safely out of reach of children and the elderly, as taking these can cause harm to them.
-
How do I dispose of extra opioid medication?
If you have unused opioids, most pharmacies in British Columbia have a drug return program where they will properly dispose of extra medications.
Never save medications, thinking you may use them at a later date.
All medications have expiration dates and may not be safe to take later.
Incision care
- Check your incisions every day.
- Incisions can be left open to the air.
- If you have sutures (stitches), these can catch on your clothing; if this happens, place a light dressing (like a bandage or gauze pad) on top.
- DO NOT rub creams or lotions (such as Polysporin, Vitamin E) on the wound unless your health-care team tells you.
- Cover your incision for the first year to prevent your scar from darkening, as it can be easily sunburned. Once the incision is completely healed, you may apply sunscreen to protect your incision.
If you have a sternal incision, you will notice a lump at the top. This is normal; the lump will gradually flatten over the coming weeks.
It is common to notice areas of numbness around an incision after the nerves in the skin have been cut. Nerves take a long time to grow back. The numbness may take months to get better, and in some cases, it may be permanent.
Sometimes, a small amount of clear, yellow, or reddish-coloured fluid may leak from your incision. This usually goes away after a few days. If it starts to leak at home or has not stopped by the time you leave the hospital, you or a family member will be taught how to apply and change dressings until the leak stops. Community nurses may help you if the incision care required is more complex. The health-care team will organize this before you leave the hospital.
If the incision starts to leak at home, you can place a dressing on top and change it daily until the leak stops.
Please call your primary care provider if you notice:
- The drainage (fluid) is thick yellow-green or cloudy
- A red, tender area in your incision that is warm to the touch
- New swelling or a sharp pain in your incision
- Fever
Washing
- Keep your incision and dressings as dry and clean as possible.
- You started having showers in the hospital and may shower after you go home (even with staples in place) if you can sit/stand safely, unless told otherwise.
- Soap and water can run over the incision.
- Pat your incision dry with an unused and clean towel (do not use the towel you used to dry your whole body).
- DO NOT directly spray water or soap over the incision.
- DO NOT rub your incision.
- DO NOT soak in a bath, pool, hot tub, or lake until your health-care team or primary care provider says it is safe.
As your incision heals, it may become itchy. Avoid rubbing or scratching. Itchiness is a normal part of the healing process.
Strips of tape called “steri-strips” may have been used to assist in securing your incision(s). If the tape gets wet, pat it dry. The tape will fall off around six to 10 days after leaving the hospital.
Slight numbness, swelling, tingling, bumpiness, firmness, and discolouration around the incision site are normal after surgery, and will improve with time. If this persists with no improvement, inform your surgeon or primary care provider.

This video has subtitles in multiple languages. Please click on the wheel icon (settings) at the bottom right of the video player, click “Subtitles,” and then choose from the list of languages.
Diet
Good nutrition speeds up healing and lessens fatigue. It may take some time before your appetite returns to normal. Your body will need extra calories, nutrients, and protein to heal.
When you attend the Cardiac Rehabilitation Program, you will have the opportunity to see a registered dietitian and have your diet reviewed and adjusted as needed for long-term health.
Below are general guidelines. Please follow the specific instructions given to you by the health-care team.
- The diet you follow at home is essential to your recovery and general health. Resume your usual diet at home. For two months after your surgery, you must eat a regular diet for the nutrients required for healing. Afterwards, you should return to a cardiac diet (low-salt and low-saturated fat diet).
- You need extra protein while you are recovering. Try to eat high-protein food at each meal and snack. Examples are chicken, beef, wild game, fish, eggs, tofu, lentils, nut butter, peas, and beans. Dairy products such as milk, yogurt and cheese are also good protein sources.
- Your fluid intake may be restricted to one-and-a-half litres per day to help prevent fluid retention and swelling in your legs.
- If you cannot eat much, make sure the fluids you choose are high in protein (e.g., soup with meat or legumes, milk or soy milk, smoothies made with yogurt, tofu, or protein powder). Another option is drinking one or two nutrition supplement drinks (e.g. Boost® or Ensure® or no-name alternatives) each day.
- If your meals are smaller than average, add one to two snacks daily.
- If you experience discomfort with chewing or swallowing, take your pain medication 30 minutes before meals.
- If your health-care team or dietitian has recommended that you follow a specific diet, please follow it as directed or until you follow up with your surgeon.
- Your dietitian will provide education and handouts if you go home on a new diet.
If you have questions about your nutrition, contact HealthLink BC by dialling 8-1-1 and ask to speak to a registered dietitian (9 a.m.–5 p.m. Monday to Friday). Make sure to mention that you have had surgery.
Managing daily activities
Sleep
It is normal to have difficulty sleeping when you first get home. This will improve with time. If you have discomfort and difficulty finding the proper position to sleep in, taking pain medication (i.e. Tylenol) may be helpful before going to sleep.
If you do not feel tired, have difficulty falling asleep or wake up throughout the night, you may sleep too much during the day. Keep your naps short and avoid napping late in the day. Stay as active as possible, spending most of the day out of bed. Avoid caffeinated drinks late in the day.
Relaxation and meditation exercises are also helpful to promote sleep.
If you continue to have difficulty sleeping, taking a sleeping pill short-term in the first one to two weeks after you leave the hospital may be helpful. Talk to your health-care team about whether or not a sleeping pill would be appropriate for you.
Sternal precautions
If you had your sternum (breastbone) cut, it will take eight to 12 weeks to heal. Stainless steel wires are placed during surgery to help hold your sternum together until the bone is healed. The wires stay in place long-term.
To help your sternum heal, AVOID:
- Lifting, pushing or pulling anything heavier than five to 10 pounds (i.e. groceries, laundry, children, pets, garbage).
- Using only one arm to push or pull.
- Reaching behind your back or above your head.
- Reaching or stretching your arms out to the side more than 90 degrees.
- Sleeping on your stomach.
- Coughing without supporting your chest.
Getting dressed
- Slow down and think about your movements.
- Keep your arms in front of you.
- Larger short sleeve shirts will be easier to put on and take off.
- Sit down to put your underwear and pants on over your feet, then stand up to pull over hips.
- Put your belt through the pants loops before putting your pants on.
- Having a Shower
- You may need help to wash your back.
- Avoid pushing or pulling on grab bars.
- Do not stay in the shower too long.
- Always raise and lower both arms at the same time when moving your arms above shoulder height. (e.g. to wash or comb hair)
Using the Toilet
- Do not hold your breath when having a bowel movement. Relax and breathe.
- Do not reach behind you.
- Wipe from the side or front.
- Stand up and face the toilet to flush.
Note: You may need a raised toilet seat or a bath transfer bench at home for a short time after surgery. The occupational therapist will assess this following your surgery.
Riding in a Vehicle
- Use a stool to enter pick-up trucks or other high cabs.
- Sit on the seat first, and then swing your legs in.
- Reach across your body with your left hand to put on your seatbelt.
- Place a pillow between your chest and seatbelt if it is more comfortable.
For people with larger breasts, wearing a bra will help to prevent the breasts from pulling at the chest incision. A front-closing bra without an underwire is recommended. If the bra rubs the incision, you can put a piece of gauze between the bra and your incision to prevent contact.
You may experience clicking sounds in the chest with specific movements or activities while the sternum is still healing. These sounds are made by movement in the sternum. An occasional click is normal but call your surgeon's office if it starts happening more often and you develop more pain or movement in the sternum. Frequent clicking may be a sign that some of the wires are broken. Avoid movements that cause clicking.
The health-care team will advise you about when you may return to normal activities.
General Guidelines:
- After eight weeks - return to normal activities
- After 12 weeks - return to normal activities involving heavy lifting
Ask the health-care team or your primary care provider if you have any questions about when you can go back to activities related to your specific needs.
Sexual Activity
Some people find they do not have the same interest in sex as they had before surgery. This is normal, and interest usually increases as you feel stronger. You can resume sexual activity when you think you have enough strength and your pain is under control. If you have difficulties, more time may be required. If problems persist, speak to your primary care provider.
Sexual activity uses the same energy as climbing up two flights of stairs at an average pace. When you can climb two flights of stairs without getting tired or short of breath, you may return to your regular sexual activity.
Do not use positions that put pressure on your chest or need support from your arms. Use a position that you and your partner find comfortable.
Try not to have sex after a large meal or exercise. If you feel tired or tense, wait until you are more rested.
Driving a car
When you can resume driving a car depends on the type of surgery you had and how well you are recovering. ICBC guidelines state that if you had coronary artery bypass surgery or valve surgery, you may resume driving one month after your surgery. Your health-care team will discuss recommendations regarding driving a car before you leave the hospital.
Before driving, check with your doctor to ensure it is okay. Only drive if you can:
- Put pressure on the brake quickly and without pain.
- Safely do a shoulder check.
- Wear your seatbelt.
- Focus and pay attention.
Opioid pain medications can impair your driving. Do not drive until you are no longer taking opioids. Always read and follow any instructions provided with your medications. If you have questions, discuss them with your doctor or pharmacist. If you are a commercial driver, please ask your doctor for permission before resuming commercial driving. In general, commercial drivers may not drive for three months.
Going Back to Work
After surgery, you will be quickly tired and may have difficulty concentrating. This is normal and will improve. Always check with your health-care team or primary care provider before returning to work. Some people return to work six to 12 weeks after surgery. When you go back to work will depend on your work and the type of surgery you had. Sometimes, it can take longer for you to recover enough to go back to work.
Resources
-
-
Heart and Stroke Foundation: recovery and support
Information for people with heart disease and their families.
-
Pacific Open Heart Association
The Pacific Open Heart Association is made up of people from BC and the Yukon who have had heart surgery.
-
Heart Hub: For patients/by patients
-
The Society of Thoracic Surgeons
-
Pain BC: Resource for pain management
-
HealthLink BC
Non-emergency health information provided by a nurse, pharmacist or dietitian.
-